


025 Ultrasound Guided Procedures & Nerve Blocks - (General Safety & Logistics)
1 February 2022
https://anchor.fm/jonathan-wallace-md/episodes/Ultrasound-for-Procedures--Nerve-Blocks-Safety--Logistics-e1dd9ut
Comments? Questions? Drop us a message!

024 PE Case
Published 25 January 2022:
https://anchor.fm/jonathan-wallace-md/episodes/Massive-PE--Thrombolysis-with-Dr-Natasha-Goumeniouk-e1dh3bi
Comments? Questions? Drop us a message!

023 Shock Overview
Published: 9 Jan 2022
https://anchor.fm/jonathan-wallace-md/episodes/Shock-Overview-e1coa7h
Comments? Questions? Drop us a message!

021 & 022
Bronchospasm Catastrophe
Published 24 December 2021:
Part A: https://anchor.fm/jonathan-wallace-md/episodes/Bronchospasm-Catastrophe-Part-A-e1c4u5q
Part B: https://anchor.fm/jonathan-wallace-md/episodes/Bronchospasm-Catastrophe-Part-B-e1c6526
Comments? Questions? Drop us a message!

020 Pseudo-Paralysis
Published 4 December 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Pseudo-Paralysis-e1b7mr6
Comments? Questions? Drop us a message!

019 Cardioversion
& Demand Ischemia
Published 27 November 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Cardioversion-for-Demand-Ischemia-e1ap109
Comments? Questions? Drop us a message!

018 (Bonus!) Lung Ultrasound
Should CXR Belong in a museum?
Published 06 November 2021:
Watch the recording on:
-- vimeo.com: https://vimeo.com/643052970 or
-- embedded below
Comments? Questions? Drop us a message!

017 Cardiogenic Shock Case
Published 23 October 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Cardiogenic-Shock-Case-with-Dr-Vanessa-Rogers-e18sr0n
Comments? Questions? Drop us a message!
Initial Scan
Follow Up Scan
(~10 days later)

016 (BONUS!) straight forward Intubation + Ventilator Case
Published 16 September 2021:
https://anchor.fm/jonathan-wallace-md/episodes/BONUS--straight-forward-Intubation--Ventilator-Case-e18ssnk
Comments? Questions? Drop us a message!

015 Anesthetic Drug Choices in the Rural Emergency Department
Published 2 October 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Anesthetic-Drug-Choices-in-the-Rural-ER-e187q9t
Comments? Questions? Drop us a message!

This table is provided as a sample based on personal experience.
Exact numbers and properties will vary depending on the source.

014 LPs (Part 2) CSF Orders + Testing Thresholds
Published 27 September 2021:
https://anchor.fm/jonathan-wallace-md/episodes/LPs-Part-2-CSF-Orders--Case-conclusion--Testing-Threshold-e17ahqs
Comments? Questions? Drop us a message!

013 Lumbar Punctures (Part 1)
Published 18 September 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Lumbar-Punctures-Part-1-e17a39q
Comments? Questions? Drop us a message!

012 Successful Sim, Rural Resuscitation & Checklists
Published 11 September 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Successful-Sim--Rural-Resuscitation--Checklists-e177u9p
Comments? Questions? Drop us a message!

011 Procedural Maintenance
Published 28 August 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Maintenance-of-Procedural-Competence-e156e33
Comments? Questions? Drop us a message!

Published 14 August 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Baking-Soda-Poisoning-e1525lj
Comments? Questions? Drop us a message!

Published 31 July 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Difficult-Airway-e13sss5
Comments? Questions? Drop us a message!

Published 24 July 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Pharmacological-Restraints-e13ssrh
Comments? Questions? Drop us a message!
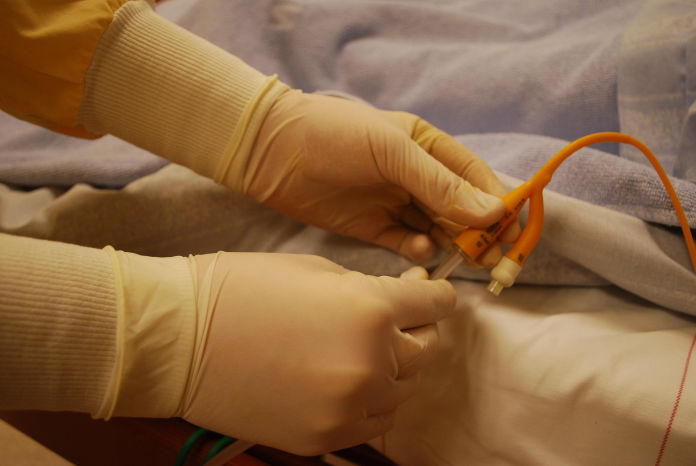
Published 17 July 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Suprapubic-Catheter-e13ssn1
Comments? Questions? Drop us a message!

Published 9 July 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Cold-Foot-e13ssll
Comments? Questions? Drop us a message!
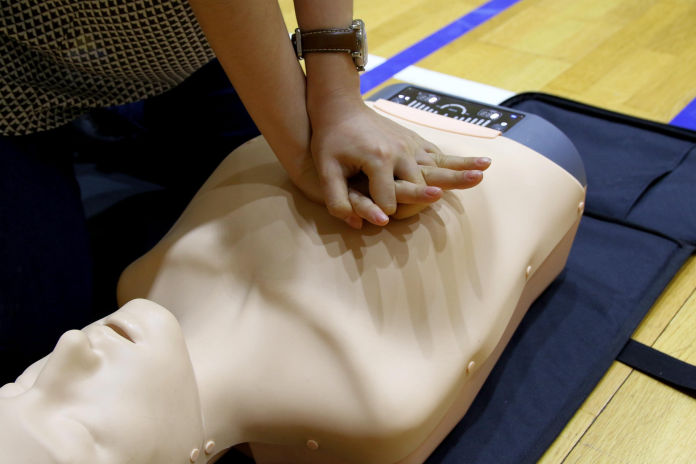
Published 3 July 2021:
https://anchor.fm/jonathan-wallace-md/episodes/PEA-e129qr4
Comments? Questions? Drop us a message!

Published 26 June 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Back-Pain-e129qms
Comments? Questions? Drop us a message!
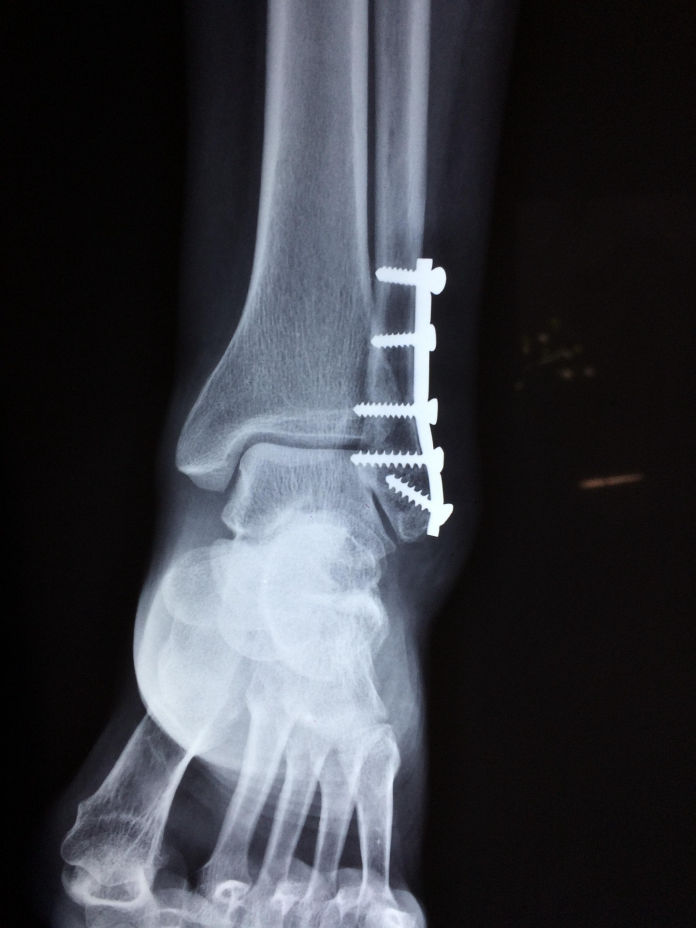
003 Ankle Fracture Reduction
Published 19 June 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Ankle--Reduction-e129qke
Comments? Questions? Drop us a message!

Published 6 June 2021:
https://anchor.fm/jonathan-wallace-md/episodes/Geriatric-Confusion-e129f9t
Learning Objectives:
POCUS: bladder volumes:
☙ Volume = (Length x Width x Depth) ÷ 2
☙ more sophisticated formulae exist (and are a possible barrier to using?)
⁍ ask yourself: will accepting a small estimation error of the simple formula affect your clinical decision making?
1. Screening & definitions for suspected sepsis:
☙ SIRS (systemic inflammatory response syndrome) - need 2 or more: to meet "SIRS Criteria":
⁍ Temperature > 38ºC or < 36ºC
⁍ HR > 90
⁍ RR > 20 or PaCO2 < 32
⁍ WBC > 12 or < 4 or >10% band cells
☙ Sepsis Criteria = SIRS + suspected infectious source
☙ Severe Sepsis = sepsis criteria + one of:
⁍ lactic acidosis
⁍ Systolic Blood Pressure (SBP) < 90
⁍ SBP > 40 below chronic baseline (e.g. 150 -> 100)
☙ qSOFA (quick sequential organ failure assessment) - need 2 or more to predict higher mortality:
⁍ GCS < 15
⁍ RR > 22
⁍ SBP < 100
2. Management priorities for suspected sepsis:
☙ Too much IV fluid can be as bad as too little fluid
☙ POCUS will lend more precision in ordering fluids
⁍ consider scanning one or more of:
⁍ inferior vena cava ●(beginner)
⁍ lungs [for B-lines, effusions] ◾️(intermediate)
⁍ left ventricular function [PSL,A4C,S4C] ◾️
⁍ emerging standard? VEXus Scan ⬥⬥(advanced!)
☙ Order cultures (blood, ±urine, ±sputum, ±CSF, etc) as soon as the possibility of sepsis enters your brain.
⁍ Cultures aid antibiotics down the road, but delaying antibiotics = increasing mortality. Do not delay antibiotics to obtain cultures.
☙ early antibiotics:
⁍ lots of good options, depending on suspected source (or lack thereof). e.g. one or more of: piperacillin-tazobactam, ceftriaxone, imipenim, amoxicillin-clavulinic acid, ciprofloxacin + metronidazole, and more.
⁍ add vancomycin (immunocompromise suspected)
☙ Surviving Sepsis Campaign offers international guidelines. 2016 was the most recent (accepted) release.
⁍ RnR Rounds Infographic on 2016 SSC Guidelines
3. Have a very low threshold to hold / observe elderly, really young (e.g. < 3 mos), frail or suspected immunocompromised patients.
Comments? Questions? Drop us a message!

Published 6 June 2021:
https://anchor.fm/jonathan-wallace-md/episodes/RnR-Rounds-Podcast-Intro-to-Series-e129eug
Target Audience For this Podcast:
☙ Rural Generalists covering their local Rural Emergency Department (usually part time ER Physicians)
PODCAST Objectives:
☙ Primary goal is discussion of real life RURAL RESUSCITATION cases
☙ Canada's Emergency Physician training [CFPC 2016]:
⁍ 55% GPs (e.g. CCFP) ← target audience!
⁍ 35% GP+extra training (e.g. CCFP-EM)
⁍ 10% specialist Emergency Physicians (e.g. FRCPC)
Do you know a Fort St Nowhere?
☙ fictional, prototypical Canadian rural/remote hospital
☙ GP-run hospital, occasionally cut off by weather
☙ ~ 12 inpatient beds ± maternity program
☙ Emergency Department with 1-2 RNs, and single physician coverage
☙ Diagnostics & Imaging In Community:
⁍ POCUS (Point of Care Ultrasound) 24hrs
⁍ Plain-Films
⁍ On-site Lab with 4 units of PRBCs
☙ Visiting surgeon, GP-ESS ± GP-Anesthetist
☙ Several hours' drive to closest regional hospital with:
⁍ closest CT Scanner & advanced diagnostics
⁍ most core specialty services.
Other Great Podcasts for Rural Generalists in the ED:
☙ EMCRIT - bleeding edge resuscitation & critical care education (aimed at tertiary care level)
☙ CrackCast - review of Rosen's Emergency Medicine textbook (FRCPC exam prep)
☙ Broome Docs Podcast - rural GP discussing emergency medicine EBM with colleagues
Comments? Questions? Drop us a message!